Medical professionals continue to worry about a problem that’s just as big as the pandemic
Content warning: Addiction, mental health, overdosing and excessive drug use.
As COVID-19 continues to concern Canadians, another threat has medical professionals worried: the opioid crisis.
Between April and June 2020, there were over 1,628 opioid toxicity-related deaths, resulting in a startling 54 per cent increase from the year before. Nearly 97 per cent of these deaths were found to be accidental.
One of the major players leading to this high death toll is fentanyl. Normally used for pain management, this highly potent drug is often mixed with other drugs like heroin, cocaine, and marijuana for a stronger high.
As a result, it makes it very easy for people to overdose, which is why 75 per cent of opioid toxicity deaths in Canada in 2020 were linked to fentanyl. This is additionally concerning as a new yellow fentanyl has appeared in Brockville and Smiths Falls.
Sonya Lockyer, the CEO of Canadian Treatment Centres, referred to this crisis in an interview as a “poisoning crisis.”
“It’s not just an overdose crisis; people don’t know what is in the drugs they are taking and often don’t have a choice because safer options are not available to them,” she said.
“We’re currently battling an epidemic within a pandemic.”
The result of more potent drugs and a nationwide lockdown created a dangerous combination for opioid users. Lockyer attributes the high number of fatalities to various reasons, but boiled it down to three prime factors; mental health, lack of oversight and access to hospital services, and the stronger substances on the market.
Mental health during the pandemic has proven to be difficult for many Canadians, especially for people with substance use disorders. According to a survey by the Mental Health Commission of Canada, one in two Canadians with underlying substance use disorders reported moderate to severe symptoms of depression since March 2020.
Lisha Di Gioacchino, a knowledge broker for the Canadian Centre on Substance Use and Addiction, believes the increase is due to strict social distancing guidelines.
“Increased isolation leads to increased opioid toxicity fatalities,” she said. “One of the main harm reduction measures is to have someone with them when they’re using a naloxone kit. So when people are in isolation, they’re less likely to use it with others. They’re also less likely to be checked in on and less likely to have access to naloxone (from harm reduction centres).”
One of the main reasons Lockyer attributes this increase in fentanyl and stronger substances, is disruptions in the drug industry. COVID-19 affected drug imports and caused drug shortages in the legal market was felt by the illegal drug market, she concluded.
Because of this, many drug dealers resorted to creating synthetic replacements to add to ‘drug cocktails,’ which includes fentanyl, heroin, methamphetamines, marijuana, etc.
The United Nations Office on Drugs and Crime noted that there have been disruptions on drug trafficking in a 2020 report, including the import of opium derived products due to air traffic disruptions. They also write that most opiate and heroin trafficking in the Americas are now done internally, creating synthetic opiates on hand has become easier and cheaper.
“Everyone’s become a chemist all of a sudden,” Lockyer said. “When you consider quality control in the illicit drug trade, it does not exist. Dealers are not in the business of killing their clients, but are often creating cocktail drugs that are deadly. Our patients sometimes learn they are taking fentanyl for the first time when they overdose or when they show up to start treatment.”
Di Gioacchino calls these mixtures “designer drugs” or novel psychoactive substances, and points to them as the illegal market’s solution to the difficulty of trafficking drugs during the pandemic.
Colleen MacPhee, the director of addiction and mental health at Rideauwood Addiction and Family Services, agrees with the fact that many of these overdoses are completely accidental and a symptom of a more toxic drug supply.
“They never had an intent to overdose, they were just using what they normally used,” she explained. “But there’s an absence of a safer illegal drug supply.”
Lockyer also points out how the lockdown has negatively impacted drug users. “The concept that the pandemic has forced people into isolation, their mental health is suffering as a result of it, and self-medication is an answer,” she said.
“Anecdotally, there’s no doubt that our patients are suffering more because of lack of services, lack of access to loved ones, and the stress of the pandemic and as a result, there’s lots of instability in our patient base, more than we’ve ever seen.”
She adds that she’s seen many missed doses and relapsing throughout 2020. Gerry Schmidt, chief operating officer of Valley Healthcare Systems in West Virginia, agrees with this, saying he’s seen a similar trend. However, he notes this isn’t a new phenomenon.
“It comes in trends, heroin was a big deal in the early 70s, post-Vietnam War all those young women and men coming back from Vietnam addicted to heroin. Then we saw LSD, then you saw cocaine became an issue then methamphetamines, crack and then pot. And now we have heroin again,” he said.
“It’s driven by demand, if you don’t decrease the demand then you really won’t stop the flow. It’s a vicious cycle really.”
MacPhee touches on this “heartbreaking” reality.
“Some of them are caused by just using them alone. People used to be able to check on you and knock on your door and they have a naloxone kit. That socialization was really important.”
Lockyer also adds that the stigmatization of drug use has further pushed people into isolation. “No one wants it in their neighbourhood [or] ‘not in my backyard.’ So that further stigmatizes these people.”
The beginning of the pandemic also saw a drop in hospital visits related to overdoses or mental health-related incidents. Lockyer believes this to be due to the fear of getting COVID-19 in the early days of the pandemic.
“People were scared, they had to choose ‘do I go to the hospital or do I stay at home’ and they stayed at home and dealt with it alone.” But she says she’s been seeing a rebound in cases.
MacPhee adds to this, saying that she’s seen an increase of people coming into her clinic later in 2020 and currently. “We’ve seen a significant increase now with people who are reaching out for help with addiction and substance use.”
“We have people calling us now who are alone, isolated, probably not noticing how they were doing with their addiction and people who had been substance-free or been in recovery have had issues with relapsing because of the loneliness and isolation,” she said.
“They used to have access to more support, and now all of a sudden they’re on their own. And then if they had mental health issues it would then be a bit more intense trying to deal with that by yourself.”
Lockyer believes the future will be quite grim if nothing is done to fix the growing problem of opioid use nationwide. She estimates a lower overall life expectancy in the country, and the impact will soon touch everyone in Canada.
“Just because a person uses drugs does not mean their life doesn’t count. The grieving associated with parents losing children does not change when it is drug use because of their loss. The grief and the mourning in our communities is tangible, you cannot open a paper these days without reading about the tragic loss this crisis is causing,” she said.
“It’s just a matter of time given where the death rates are going that everyone will be impacted by this crisis. Even now, most people I speak to know someone who has a problem with opioid use.”
She adds to this by saying her current concern of temporarily stopping the epidemic is the long-term impact we’ll be seeing on users. The key is educating and de-stigmatizing substance use.
“Many of these prescription opioids are now ending up on the street for resale. Our fear is that while we may be reducing overdose deaths in the moment, we may also be contributing to the next wave of the opioid epidemic?”
Schmidt also emphasizes the importance of education, especially for young people and children when combating the stigma and spreading information around substance use disorders.
“We need to get people to understand it can be corrected, it can’t be cured, but going forward we need to educate more especially early on,” he said.
“We have to remind people that these drugs may temporarily make you feel better but it won’t correct the problem. I hear from patients that using drugs was the first time in their life they felt normal. We need to show there is a way to achieve that without introducing drugs into their system.”
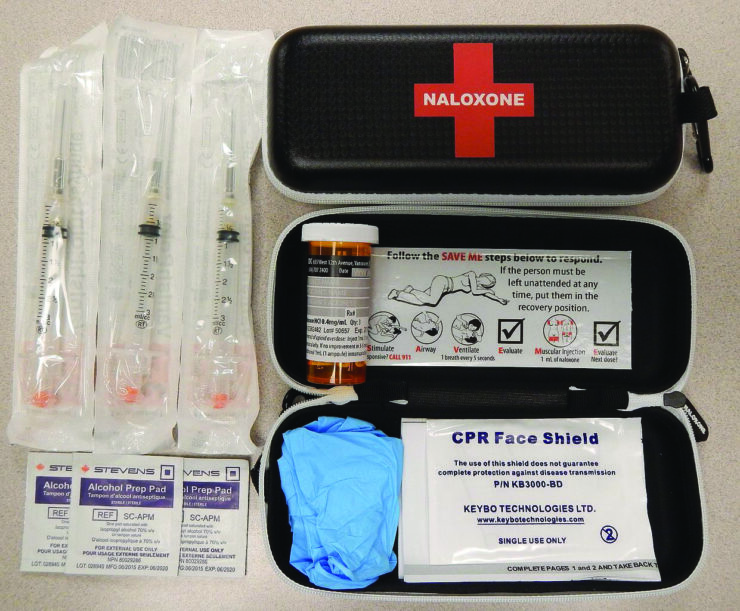
One of the first tips, MacPhee adds, is to teach more of the population whether in the healthcare field or not, about a naloxone kit as they can be the key to saving someone’s life if they have an overdose.
“We need to be educating the public more on (naloxone) kits, especially if there could be someone in your life who could be or have a history of using,” she said.
“Get a naloxone kit, just have it in case you need it. You hope you never have to use it but if you do, you have access to it.”
Below is a provided list of resources for addiction treatment
- Mental Health Committee of Canada
- Tel: (613) 683-3755
- Email: mhccinfo@mentalhealthcommission.ca
- Ontario Addiction Treatment Centre
- Tel: (905) 773-3884
- Email: info@canatc.ca
- Rideauwood Addiction and Family Services
- Tel: (613) 724-4881
- Canadian Centre on Substance Use and Addiction
- Tel: 1 (833) 235-4048