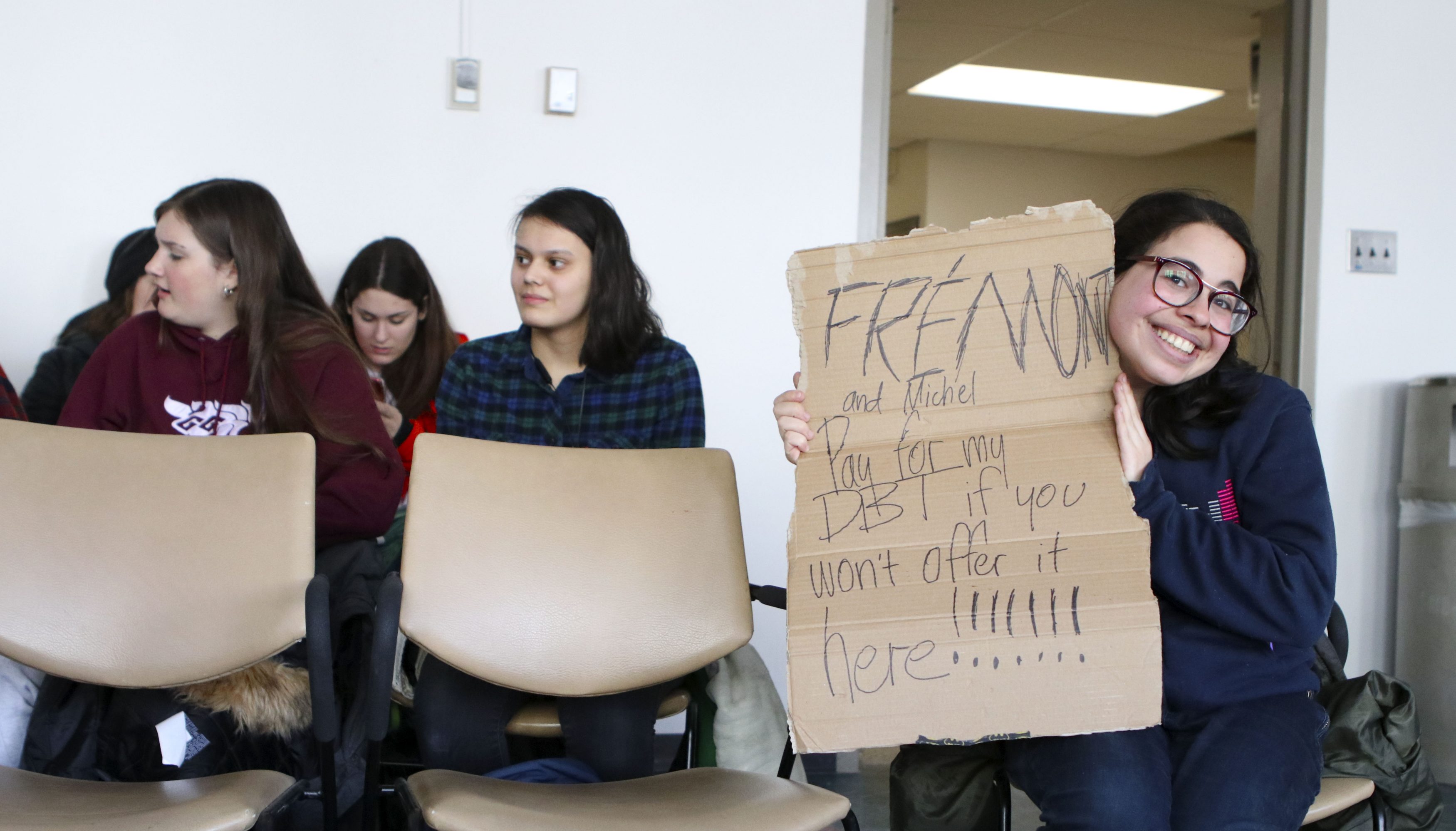Students highlight anti-psychiatry exhibit, need for mental health training for professors at town hall for faculty of arts
Content warning: Suicide
Several University of Ottawa students pushed for immediate action on improving the school’s mental health system at a town hall discussion for the faculty of arts on Wednesday, with many asking president Jacques Frémont for concrete next steps on how he plans to address the situation.
The town hall comes just days after a student death, the fifth to occur in the past 10 months. During a Tuesday press conference, Frémont acknowledged that the school is dealing with a mental health ‘crisis’.
“This is a very difficult moment and it has been a difficult moment for many months and years, it is a very difficult file,” said Frémont at the start of the town hall, which was hosted in Simard Hall. “There have been some improvements. Is it enough? Clearly not.”
Frémont highlighted the school’s recently launched task force for mental health, which will be led by faculty of arts dean Kevin Kee. The task force is looking to engage with other universities for suggestions, partner with local hospitals, implement recommendations from a January report on wellness, and is set to hold a town hall on Feb. 27.
“It is really an exercise in, first and foremost, listening to what the community has to say,” said Frémont, who was joined by Kee, provost and vice-president (academic) Jill Scott, and vice-president (research) Sylvain Charbonneau.
While over a dozen professors and staff attended the town hall as well, students took centre stage, openly sharing their experiences with the school’s mental health system and highlighting crucial gaps they say need to be filled.
“If we’ve had five student deaths in the past 10 months, are we supposed to wait another 10 months and have another five student deaths?” asked one student.
“Are we waiting until it goes up to one death per month? I mean, you have a problem with it now,” said the student. “So what are we doing today, now, to help the students?”
In his response, Frémont said that there’s no easy fix to the problem.
“Do you think we can find psychiatrists like this lying in the street, waiting for me to call? It is more complex than that,” he said, highlighting the need to work with the provincial government.
He then reminded students that there are frontline workers that are ready to address their immediate needs, but also acknowledged the long wait times for those who are seeking long-term help.
“This is a shared responsibility with the province. This relates to the health system in Ontario,” Frémont said. “And again, we’re speaking with ministers, we’re trying to push the system. I think the government should take mental health issues very seriously.”
Student Angela Toubis argued that the crisis is in the school’s mental health care system, as opposed to saying that there’s a crisis with students and their mental health.
“I honestly think that if we change our language to mental health care, we can make a lot of change,” said Toubis, one of the co-founders of the uOCollective 4 Mental Health, which was launched after the fourth student death of 2019 in December.
“By saying we have a mental health crisis, we’re putting the blame on the victim by saying it’s the fault of the victim for having mental health issues — we need resources,” she said.
Toubis added that professors should receive training on how to become more sensitive when it comes to dealing with students and their mental health concerns.
“It’s really clear on which professors are aware of the issues and which ones are not,” she said.
Laura O’Connor, another co-founder of the uOCollective 4 Mental Health, shared her concern of student voices not being taken seriously or listened to.
“We hold protests just to be heard,” said O’Connor. “We perform pretty radical, laborious tasks just to be heard, and students come forward with suggestions and we feel like we’re talked down to.”
“It really does feel like university is a pyramid, a hierarchical structure with us on the bottom,” added O’Connor.
Another student brought up the damage they felt was caused by a Scientology linked anti-psychiatry exhibit that was on campus in the University Centre for a week in late January, which was set up just days after the school finished celebrating their annual Wellness Week.
“After such terrifying, disgusting propaganda on campus, I would have liked to see the (opposite display) the next week,” said the student. “If that’s not the idea that you share, why didn’t you try to bring forward the opposite message?”
Hundreds of students protested the “Psychiatry: An Industry of Death” display, which included panels reading “Inventing Disorders to Sell Drugs” and “Hooking the World on Drugs.” In an interview last month, Frémont called the exhibit “hurtful” and “outrageous” but refused to take it down.
“I’m requesting a formal apology for the anti-psychiatry display,” said another student to applause. “It was really harmful for someone who’s dealt with mental health (issues) their whole life to come to university, take this step, walk into the UCU and see a poster that says your needs aren’t valid, you’re not valid, and then to have the university try to brush it under the rug and ignore it.”
Frémont reiterated in his response to the students’ concerns that having the exhibit on campus was a mistake.
“That was a clear mistake. That being said, I had a long conversation with the head of the department of psychiatry, and we agreed that next year we’ll have at least four conferences on campus about psychiatry with guests coming (in),” he said.
Camelia Skaf, a second-year student living with a personality disorder, brought a sign reading “Frémont and Michel (Guilbeault, associate vice-president of student services) pay for my DBT (dialectic behaviour therapy) if you won’t offer it here” to the town hall.
Skaf highlighted systemic barriers to accessibility for someone with an invisible disability or a chronic illness, including mandatory class attendance and professors not using Bright Space.
“The (person) who just died could have easily, easily, easily, easily been me,” said Skaf. “Do better by us, care for us better.”
Kee asked that all students in attendance leave their name and contact info with him, so that he could invite them to the Feb. 27 town hall on mental health, where they can further share their concerns.
“We need to discuss this in detail. I need to listen and the people around me here need to listen,” he said. “There’s going to be several conversations. But that’ll be the place for us to do it.”
Students held a sit-in outside Frémont’s office in Tabaret Hall on Wednesday, organized by the uOCollective 4 Mental Health, where he met with protesters and agreed to bring them to Queen’s Park if he looked to the province for funding.
Another protest is planned for Friday on Tabaret Lawn from 9 a.m. to 12 p.m., with talks of more protests taking place after reading week, which starts this Monday.
More to come.
A non-comprehensive list of local mental health resources appears below…
On campus…
- University of Ottawa Health Services (UOHS), 100 Marie-Curie Private
- Offers counselling, psychiatric services, individual, couple or family therapy, access to psycho-educational groups and referrals to specialists off-campus
- Student Academic Success Service (SASS), 100 Marie-Curie Private
- Offers individual counselling, peer-counselling, workshops, online therapy and group counselling using new stepped model; referrals
- Faculty mentoring centres (locations differ by faculty)
- Specialized mentoring services catered to the needs of students in each faculty
Off campus…
- Mental health hotlines…
- Drugs and Alcohol Helpline: 1-866-531-2600
- Canada Suicide Prevention Service phone available 24/7: 1-833-456-4566
- Fem’aide: 1-877-336-2433
- Good2Talk: 1-866-925-5454
- Kids Help Phone: 1-800-668-6668 or text CONNECT to 686868
- Mental Health Crisis Line: 613-722-6914
- Distress Centre of Ottawa and Region: (613) 238-3311
- Ottawa Rape Crisis Centre: 613-562-2333
- Tel-Aide Outaouais: 613-741-6433
- Trans Life Line: 1-877-330-6366
- Walk-in counselling clinics (six Ottawa locations)…
- Somerset West Community Health Centre (55 Eccles Street)
- South-East Ottawa Community Health Centre (1355 Bank Street)
- Family Services Ottawa (312 Parkdale Avenue)
- Jewish Family Services of Ottawa (300-2255 Carling Avenue)
- Ottawa Community Immigrant Services Organization(959 Wellington St. W)
- CFS/SFC Ottawa (310 Olmstead Road)
- Community health and resource centres (13 in Ottawa)
- Carlington Community Health Centre (900 Merivale Road)
- Eastern Ottawa Resource Centre (215-1980 Ogilvie Road)
- Nepean, Rideau and Osgoode Community Resource Centre (1547 Merivale Road, Unit 240)
- Rideau-Rockcliffe Community Health Centre (225 Donald Street)
- Sandy Hill Community Health Centre (221 Nelson Street)
- South East Ottawa Community Health Centre (1355 Bank Street)
- Western Ottawa Community Resource Centre (2 MacNeil Court)
- Centretown Community Health Centre (420 Cooper Street)
- Lowertown Community Resource Centre (40 Cobourg Street)
- Orleans-Cumberland Community Health Centre (240 Centrum Boulevard)
- Pinecrest-Queensway Community Health Centre(1365 Richmond Road)
- Somerset West Community Health Centre (55 Eccles Street)
- Vanier Community Service Centre (270 Marier Avenue)
Warning signs of suicide include:
Talking about wanting to die
Looking for a way to kill oneself
Talking about feeling hopeless or having no purpose
Talking about feeling trapped or being in unbearable pain
Talking about being a burden to others
Increasing use of alcohol or drugs
Acting anxious, agitated, or recklessly
Sleeping too little or too much
Withdrawing or feeling isolated
Showing rage or talking about seeking revenge
Displaying extreme mood swings
The more of these signs a person shows, the greater the risk. If you suspect someone you know may be contemplating suicide, you should talk to them, according to the Canadian Association for Suicide Prevention.